Freely Available British and Irish Public Legal Information
[Home] [Databases] [World Law] [Multidatabase Search] [Help] [Feedback]
England and Wales High Court (Queen's Bench Division) Decisions
You are here: BAILII >> Databases >> England and Wales High Court (Queen's Bench Division) Decisions >> Lesforis v Tolias [2018] EWHC 1225 (QB) (21 May 2018)
URL: http://www.bailii.org/ew/cases/EWHC/QB/2018/1225.html
Cite as: [2018] EWHC 1225 (QB)
[New search] [Printable PDF version] [Help]
QUEEN'S BENCH DIVISION
Strand, London, WC2A 2LL |
||
B e f o r e :
____________________
| Yvonne Lesforis |
Claimant |
|
| - and - |
||
| Christos Tolias |
Defendant |
____________________
for the Claimant
Mr Philip Havers QC (instructed by Hempsons Solicitors) for the Defendant
Hearing dates: 16, 17, 18, 19 and 23 April 2018,
____________________
Crown Copyright ©
- On 27 June 2013, the Claimant, Mrs Yvonne Lesforis underwent spinal surgery at the hands of the Defendant, Mr Christos Tolias, a consultant neurosurgeon.
- Towards midday on 29 June 2013, Mrs Lesforis began to suffer neurological deficit in the form of inability to move her ankles and toes with a consequent inability to walk or weight-bear. Further exploratory surgery was carried out by Mr Tolias at midnight on the night of 29 June 2013, but this failed to relieve Mrs Lesforis' neurological deficit, and she has been left with serious residual and permanent disability in the form of incomplete paraplegia.
- In this action, Mrs Lesforis seeks damages from the Defendant for allegedly inappropriately early prescription of antithrombotic medication and alleged delay in carrying out the remedial surgery. This judgment is in relation to the issues of breach of duty and causation.
- Mrs Lesforis was born on 26 November 1956 and worked as a college lecturer, teaching Health and Social Care and Childcare and Education courses.
- In 2007 she started to experience significant discomfort in her lower back with pain radiating down to her calves. She went to see her GP who referred her to the acute back pain service, part of Maidstone and Tunbridge Wells NHS Trust and she was referred for physiotherapy. An x-ray in August 2007 revealed spondylolisthesis whereby an intervertebral disc slips and overlaps with an adjacent disc, thereby narrowing the spinal canal causing stenosis.
- Mrs Lesforis was referred to Mr Slater, a consultant orthopaedic surgeon at Maidstone Hospital whom she saw in the autumn of 2007. He explained that there was degeneration of the spine at the L3/4 level and although the possibility of surgical intervention was discussed, it was not recommended at that stage. In fact, thereafter, the symptoms became less severe and no further intervention was necessary.
- In about May 2009, the lower back pain symptoms increased with aching, cramping pain radiating to both buttocks and down the back of her legs. The symptoms started to interfere with her work as a lecturer and she was again referred for physiotherapy at Preston Hall Hospital. This did not help greatly and in December 2009 she was seen at the chronic pain clinic at Pembury Hospital where facet joint injections were recommended. These were performed in July 2010. Again, they were ineffective in relieving her pain.
- On 8 March 2011, Mrs Lesforis was seen by a neurologist, Dr Naheed Khan. She diagnosed radicular back pain and in particular compromise of the L4 nerve root on the right. She advised weight loss and arranged for a repeat MRI of the lumbar spine in order to identify whether there were any specific nerve root lesions, planning, on receipt of the imaging, to arrange for review by the spinal multi-disciplinary team at King's College Hospital ("KCH") London for a definitive answer as to whether Mrs Lesforis would be amenable to surgery.
- A MRI scan carried out on 22 April 2011 identified severe spinal stenosis at L3/4 but it was not clear whether the L4 or L5 nerve roots were compromised. Dr Khan reviewed Mrs Lesforis on 25 October 2011 and referred her to the spinal multi-disciplinary team at KCH. The team reviewed the case on 22 December 2011 and recommended a neurosurgical out-patient appointment. This led to the Claimant being seen by the Defendant, Mr Tolias.
- Mrs Lesforis saw Mr Tolias at KCH on 7 March 2012 who recorded that she had in fact improved since seeing Dr Khan and had very little pain that day. Mr Tolias wrote to Mrs Lesforis' GP in the following terms:
- Mr Tolias reviewed Mrs Lesforis on 12 September 2012 and he again wrote to her GP as follows:
- Mrs Lesforis decided to take up the offer of decompression surgery and she saw Mr Tolias again on 20 February 2013 who wrote to her GP as follows:
- Because of delay in having the operation done on the NHS, and being covered by private health insurance, Mrs Lesforis decided to have the operation carried out by Mr Tolias privately at the Harley Street Clinic. On 27 June 2013, she was admitted to the clinic and she was clerked in at 08.30. A CT scan of the lumbar spine was carried out and Mrs Lesforis signed a further consent form. Again, the risks of the surgery, including paralysis and loss of bowel/bladder function, were explained and acknowledged.
- The surgery was carried out by the Defendant at 13.05 hours on 27 June 2013 and apart from a minor tear of the dura at L2 level, which was recognised and dealt with at the time by being repaired with sutures, a small piece of muscle and a glue called Tisseal, the operation went smoothly and was apparently successful. Mrs Lesforis was taken to the Intensive Therapy Unit at 16.11 where hourly neurological observations were commenced and at 19.07 hours, she started a course of Low Molecular Weight Heparin, in the form of Clexane, as chemoprophylaxis against deep vein thrombosis ("DVT"). Thus, the first dose was about three hours after completion of the surgery. Because of the dural tear, Mr Tolias had ordered that Mrs Lesforis not be mobilised for 48 hours and this, together with the fact that she was overweight and had undergone surgery for more than 90 minutes meant that she was at increased risk of DVT. Although the giving of Clexane is not criticised, the timing of the first dose is.
- Mrs Lesforis was reviewed by the Defendant at 9.30 on the morning of the 28 June 2013 and he was happy with her progress. At 18.00 hours that evening, she was moved out of ITU to her own room. At that time, her clinical and neurological status were both normal.
- On Saturday, 29 June 2013, Mr Tolias visited the ward at 09.00 and was told by the nurses that all was well. He therefore revised his post-operative regime and told the nurses that Mrs Lesforis could be mobilised.
- At some stage before 12.30pm, a physiotherapist visited and tried to mobilise Mrs Lesforis. However, she noted "Patient finding difficult to WB (weight bear). Reported legs feel weak." The physiotherapist attended again at about 12.30 and this time noted:
- Another consultant neurosurgeon, Mr Al-Barazi, was at the Harley Street Clinic operating that day and Mr Al-Barazi saw Mrs Lesforis at 13.00 hours at Mr Tolias' request. Mr Al-Barazi noted as follows:
- I should say something at this stage about the fact that a CT scan and not an MRI scan was arranged. In his witness statement, Mr Tolias says that, at the time,
- Before returning to the narrative, I should also say something about the anatomy. The bundle of nerves which run down the spinal column from about the L1 level resembles a horse's tail and is referred to as the "cauda equina", as shown in this chart:
- The CT scan was carried out and the results were relayed to Dr Stephen Connor, a Neuroradiologist based at KCH. Dr Connor discussed his findings with Mr Tolias and these were later set out in a report as follows:
- In his evidence, Dr Connor explained that, having viewed the CT scan remotely, he reported his findings orally to Mr Tolias at some stage between 14.30 and 16.00, and that his written report reflects accurately what he had told Mr Tolias. He further explained that, given the clinical presentation suggesting a problem at the L5/S1 level, he was able to reassure Mr Tolias that, at that level, the CT scan gave a clear view and indicated that there was no compressive haematoma. He said:
- At a time which was probably between 15.00 hours and 16.00 hours, Mr Tolias assessed the situation, which assessment included discussion with Mr Malik and Mr Al-Barazi and also an examination of the Claimant. At 16.00 hours, he made the following note, reflecting these matters:
- felt some moderate back pain and paraesthesia down both legs
- now unable to move both feet (ankle/toes)
- able to lift both legs off bed bend hips and knees/extend both knees against gravity
- can feel catheter/wound ok
- soft tissue posteriorly (explained by Tisseal/muscle plug)
- (L) upper screw slightly medial
- D/W Mr Malik
- We cannot explain the delayed sudden bilateral distal weakness
- Levels at a distance from operative site
- Agreed to start steroids and reassess situation
- Explained problem to Mrs Lesforis and her husband. Also explained our consensus opinion and plan"
- In his evidence, Mr Tolias said that although he had discussed the matter with his colleagues, the plan and the decision as to what course to take was his alone. He said:
- In the nursing notes, there is a note made at 18:38 on 29 June 2013 in relation to Mr Tolias' review as follows:
- After his note written at 16.00 hours, Mr Tolias did not make any further entry in the medical records. However, there is a typed document dated 1 July 2013 headed "MEDICAL REPORT" which includes a passage which purports to describe the situation up to the time of re-operation. However, this document was the subject of a supplemental witness statement by Mr Tolias signed and served on 13 April 2018, the last working day before trial. In that statement, Mr Tolias says that, on 12 April 2018, he discovered that his computer still contained the dictation that became the medical report in question and a screen-shot of his computer shows that the creation of the dictation started just after 22.00 hours on 29 June 2013. Mr Tolias says that he infers from this that he started dictating the note whilst he was waiting for Mrs Lesforis to be brought to the operating theatre. The dictation was completed at 08.28 on 1 July 2013 when Mr Tolias says he sent it to his secretary to be typed. Comparison between the actual dictation and the typed "medical report" revealed some typos and omissions and therefore a revised version of that medical report has been produced. It reads as follows:
- In his evidence, Mr Tolias said that he had examined Mrs Lesforis again before taking her to theatre and having found no change in her condition, he summarised it in his dictated report. This included an examination of the anal sphincter, which was normal.
- The Claimant was taken back to theatre at 23.40 hours and Mr Tolias re-operated at about midnight. He noted the operation to be "Re-exploration of wound and clot evacuation". His operation note was contained in the continued dictation of the "medical report" dated 1 July 2013 and reads as follows:
- Mr Tolias saw Mrs Lesforis at 11am the following morning and he made the following note in her medical records:
- Post op wound exploration
- Mrs Lesforis was seen by a physiotherapist at midday on 30 June 2013 who noted, among other things:
- Mrs Lesforis was seen again by a Mr Al-Barazi at 9am on 1 July 2013 who carried out a neurological examination. He noted:
- On 2 July 2013, nerve conduction studies were carried out by Dr Ian Mak and a post-operative MRI scan was also carried out. On 16 July 2013, Mrs Lesforis was discharged from the Harley Street Clinic and admitted to Gravesham Community Hospital for rehabilitation. From there she was further transferred to Stoke Mandeville Hospital on 4 September 2013 for further expert rehabilitation and she was finally discharged on 14 February 2014. Whilst this trial is concerned only with liability issues, I note that, in a medical report dated 24 March 2015, it is reported that Mrs Lesforis has dense sacral nerve deficits with a denervated bladder and bowel. She has no sensation in the L1-L4 dermatomes bi-laterally. She manages her bladder by regular intermittent self-catheterisation. Her bladder has no sensation, nor does her bowel and she relies on an irrigation system. Her mobility is severely restricted on account of nerve root injury from L3 down to S1 affecting her knees and ankles and she also has neuropathic symptoms in her lower limbs. She is largely wheelchair bound.
- For the Claimant, it is alleged that the cause of the deterioration in Mrs Lesforis neurological condition on 29 June 2013 and thereafter was a compressive epidural haematoma, itself caused by the early administration of Low Molecular Weight Heparin ("LMWH") which had been given as chemo-prophylaxis against the formation of DVT. The formation of a compressive haematoma causing neurological symptoms is a medical emergency and requires immediate re-operation to evacuate the haematoma and relieve the pressure on the dura and its contents, the nerve roots, so as to avoid permanent neurological injury. It is the Claimant's case that, after the onset of neurological symptoms, there is a window of opportunity during which, if the problem is alleviated, there is a good chance that the nerves will recover and function will be restored. Although it is acknowledged that Mrs Lesforis might well have been left with some residual symptoms, these would have been minor compared to the devastating condition in which she now finds herself. It is alleged against Mr Tolias that, firstly, chemo-prophylaxis was given much too soon after surgery, at a time which was outside normal practise and which negligently increased the risk of haematoma formation, as occurred. Secondly, upon neurological deterioration, Mr Tolias should have arranged for a MRI scan to give himself the full picture of what was going on and in order to inform his clinical decision making. Finally, it is alleged that there was a negligent delay in re-operating. It is alleged that decompression should have been achieved by about 4pm on 29 June 2013 rather than after midnight on 30 June 2013 and this delay of eight hours or so was fatal to Mrs Lesforis' chances of recovery.
- For the Defendant, liability is denied. In relation to the giving of chemo-prophylaxis, it is agreed on all sides that this was appropriate. The only issue surrounds the timing. At the time of this operation, although there were NICE (National Institute of Clinical Excellence) guidelines, these did not give any guidance or assistance in relation to the timing of chemo-prophylaxis. It is the Defendant's case that there was a wide variation in practice and an absence of literature either telling practitioners when to give chemo-prophylaxis or establishing that the risk of post-operative haematoma is significantly increased by the giving of very early chemo-prophylaxis. Thus, it is denied that the practice of Mr Tolias in giving chemo-prophylaxis when he did can be said to be negligent within the "Bolam" test. So far as the obtaining of a MRI scan is concerned, it is the Defendant's case that he had all the radiological evidence that he needed from the CT scan that was carried out in the early afternoon of 29 June to make the management decisions required. MRI was not available as an emergency at the Harley Street Clinic (this was not his responsibility) and although he could have transferred Mrs Lesforis to a NHS hospital for a MRI examination, this would have involved delay. In any event, a MRI would not have changed the situation or caused him to act differently. Finally it is the Defendant's case that the clinical position with which he was confronted was unusual and difficult. He was told by Dr Connor that it was highly unlikely that there was a compressive haematoma at the site of his operation which was causative of Mrs Lesforis' condition. His case is that the absence of muscle movement in the ankles and toes was indicative of a problem at the L5/S1 level which was distal to his operative field and was an area of the spinal cord which was seen on the CT scan to be wholly clear of compression. Even if compression could not be wholly ruled out at the operative site, his view was that this would not explain a lesion which appeared to have selected the L5/S1 nerve roots to the exclusion of the L3/S4 nerve roots or, indeed, the S2-S5 nerve roots. He therefore justified his decision to give steroids in the form of Dexamethasone and to see whether they resulted in an improvement by treating any inflammation. After the Dexamethasone failed to produce any change at all, he then decided to re-operate, principally to explore the wound and because it was the only option left to him at that stage. However, he held out little hope of any significant improvement. He denies that it was negligent for him to fail to operate earlier than he did.
- At the trial, I heard evidence from Mrs Lesforis and also from Mr Tolias, and the other doctors involved on 29 June 2013: Mr Al-Barazi, Dr Connor and Mr Malik (with whom Mr Tolias had originally operated and with whom Mr Tolias discussed the situation on 29 June 2013). I also heard evidence from expert neurosurgeons called for each side, Mr John Leach and Mr Thomas Cadoux-Hudson. I shall deal with their evidence in more detail in relation to the issues as they arise for consideration. However, although in a case such as this I will inevitably need to decide whose evidence I prefer, I can indicate that I generally felt that all the witnesses were trying to assist the court and that both experts were impressive.
- In their opening note for the purposes of the trial, counsel for the Claimant suggested that there are three key issues for determination:
- Although the precise time of the conclusion of the operation on 27 June 2013 is not recorded, Mrs Lesforis was admitted to ITU at 16.11 and this gives an indication of the timing of the end of the operation allowing a short period of time in recovery before transfer to ITU. The first dose of Clexane was administered at 19.07 hours that evening and it is agreed between the parties that chemo-prophylaxis was therefore given within about three hours of the end of the operation.
- In his witness statement, adduced as his evidence in chief for the purposes of the trial, Mr Tolias said:
- For the Claimant, Mr Leach acknowledges there is a range of opinion on the appropriate timing of commencement of chemo-prophylaxis against venous thromboembolism. However, he is critical of the giving of Clexane that early. He says:
- For the Defendant, Mr Cadoux-Hudson states, in relation to the allegation of breach of duty in giving anti-coagulant within 12 hours of surgery:
- The neurosurgeons held a Joint Experts Meeting ("JEM") in February 2018, as ordered by the court for the purposes of discussing the issues arising in this case. Each side produced its own agenda for the purposes of the discussion. Asked the question:
- So far as the Defendant's agenda is concerned, the questions and answers provided by the experts were as follows:
- In relation to questions 2.1 and 2.2, Mr Leach confirmed that these questions related to all surgery, and were not confined to spinal surgery which is dealt with from questions 2.3 onwards.
- Both experts were cross-examined on this issue when they gave evidence. Mr Havers QC put to Mr Leach the medical literature on the subject, such as it is. Firstly, an article by Khan and others from the Journal of Neurosurgery in December 2017 conducted a meta-analysis of chemical VTE prophylaxis in neurosurgery. The authors stated:
- In addition, Mr Leach made the, as it seems to me, equally pertinent point that the Khan conclusion is not reflected in the current NICE guidelines. NICE revised their guidelines for VTE prophylaxis in 2018 and chapter 31 of the guideline deals with elective spinal surgery. The relevant recommendations are contained at paragraph 31.6 which includes the following:
- It was put to Mr Leach, taking the position as at 2013, the question when chemo-prophylaxis should be given, in particular in relation to spinal surgery, remained unclear and different surgeons would give it at different times. Mr Leach disagreed with that proposition. He said:
- Mr Havers QC also put to Mr Leach a paper by Gerlach and others from 2003, the aim of which was to determine the risk of post-operative haemorrhage during a three year period of early post-operative administration of LMWH. They concluded that early pharmacological anti-coagulation after spinal surgery using Nadroparin is safe and not associated with an increased risk of post-operative haemorrhage. However, their idea of what constitutes "early" anti-coagulation appears to be at least 12 hours after surgery because the medication was usually started at 8am the day after surgery. Given that the surgery was elective, and therefore is likely to have been during the day, finishing at latest by about 6pm, to start LMWH at 8am the following day would give an interval of 14 hours plus. Mr Leach made five points in answer to the Gerlach paper:
- For the Defendant, Mr Cadoux-Hudson was also questioned about the timing of the Clexane. Mr Aldous QC pointed out to Mr Cadoux-Hudson that he had not said in his report that he was aware of some surgeons who would routinely give chemo-prophylaxis within three hours of surgery. Mr Cadoux-Hudson answered:
- In re-examination, Mr Cadoux-Hudson was referred again to his answers at the JEM and he was asked this question:
- For the Defendant, Mr Havers QC submitted that, in prescribing Clexane for Mrs Lesforis within six hours of surgery, Mr Tolias did not act negligently relying on eight matters:
- For the Claimant, Mr Aldous QC pointed out that the experts had agreed that the timing of LMWH is a matter of clinical judgment that depends upon patient risk factors for VTE and the bleeding risk of surgery but the timing of the giving of chemo-prophylaxis in this case was not based upon a specific risk assessment for this particular patient by Mr Tolias, but was based upon his normal practice for all his spinal patients. This led Mr Aldous to be critical of a particular passage in the evidence of Mr Cadoux-Hudson where he suggested that there would have been a discussion between Mr Tolias and Mr Malik (who assisted him in the operation on 27 June 2013) about the giving and timing of chemo-prophylaxis. Mr Cadoux-Hudson had said:
- Mr Aldous QC submitted that the administration by Mr Tolias of LMWH after three hours without any consideration of the risk benefit analysis for this particular patient cannot be justified as compliant with the standard accepted by a reasonable body of practitioners or as one that withstands logical analysis. He submitted:
- In further written closing submissions, Mr Havers QC again referred to the papers by Khan and Hamidi which, he said, showed that spinal surgeons were giving chemoprophylaxis pre-operatively in 2011 prior to elective instrumental spinal surgery and if, therefore, there was a reasonable body of spinal surgeons giving it pre-operatively, then it cannot be a breach of duty, within the Bolam test, for a surgeon to give it within 6 hours post-operatively. To this, Mr Aldous responds by referring the court to the evidence of Mr Leach where he said (Day 2):
- Other arguments on each side adduced in the further submissions have been considered by me and are addressed where I consider appropriate in my discussion of this issue below.
- The resolution of this issue depends principally upon my assessment of the respective experts. In this regard, on this issue, I prefer the evidence of Mr Leach to that of Mr Cadoux-Hudson. I was impressed by Mr Leach's approach to this question and in particular his concession that if someone were to present him with evidence that there is a body of surgeons who routinely give chemo-prophylaxis after spinal surgery within six hours, for example by reference to a protocol from a respected spinal unit such as that at King's College Hospital, then he would be prepared to change his opinion. Indeed, this would have been an obvious and easy way for Mr Cadoux-Hudson to refute this allegation of negligence but he did not do so despite the fact that there are many spinal units across the country who must have protocols for the giving of chemo-prophylaxis after spinal surgery. I accept Mr Leach's evidence that he is not aware of spinal surgeons in the UK who, in 2013, were giving chemo-prophylaxis as early as within six hours of surgery and in my judgment this is likely to be because there was no such body of surgeons.
- Mr Aldous QC did not cross-examine Mr Tolias about his practice in relation to the giving of chemo-prophylaxis to his spinal patients but, in my judgment, this was because he did not need to. Mr Tolias did not suggest that he had prescribed chemo-prophylaxis to be given that evening after surgery because he had made a specific assessment of this particular patient and formed a judgement that she needed to be given chemo-prophylaxis that early. On the contrary, he suggested in his witness statement that he gave such chemo-prophylaxis that early to all his spinal patients and he did not discriminate between Mrs Lesforis and any other patient in this regard. Immediately, this raises a serious question about the practice of Mr Tolias in this regard: the experts agreed that, in relation to all surgery, the timing of prophylaxis against VTE will depend on patient risk factors for VTE and bleeding risk of surgery. The giving of very early prophylaxis to all such patients does not take into account the individual factors which need to be taken into account. It seems to me that it was for this reason that Mr Cadoux-Hudson speculated that there would have been a discussion between Mr Tolias, Mr Malik and the anaesthetist on the occasion of the first operation: as Mr Aldous put it, he speculated that this would have taken place because, in his heart, he knew it should have taken place. But it did not. When asked the question:
- I acknowledge that, at the time of this surgery, there were no NICE guidelines (as there now are) relating to the timing of chemo-prophylaxis after lumbar spinal surgery. I further acknowledge that the medical literature is poor in giving guidance on this. However, this does not preclude an allegation that the giving of very early chemo-prophylaxis falls below the reasonable standard according to the "Bolam" test. Although Mr Leach was criticised by Mr Havers QC for not having expressed himself in his report in "Bolam" terms, I accept his evidence that this is what he had in mind when he said that:
- For the reasons stated above, in my judgment it was negligent for Mr Tolias to have prescribed chemo-prophylaxis for all his cranial and lumbar patients routinely within six hours of surgery and it was negligent for him to have done so specifically for Mrs Lesforis. Mr Tolias did not explain in his witness statement the origin of this practise and that again was a surprising omission. I find that his use of LMWH after spinal surgery was cavalier, and outside the range of normal practise at the relevant time.
- For the Defendant, Mr Havers QC relies upon Mr Leach's acceptance in his evidence that there is no evidence contained in the medical literature to show that giving chemo-prophylaxis within six hours of spinal surgery increases the risk of post-operative haemorrhage. He submits that this is the starting point and the end point so far as causation is concerned. He further submits even if, contrary to his primary case, there was some causal connection between the giving of chemo-prophylaxis and the symptoms which the Claimant developed on 29 June, the first dose of chemo-prophylaxis would not have played any part in the development of those symptoms. In this regard he relies upon the evidence of Mr Cadoux-Hudson where he stated as follows:
- For the Claimant, Mr Aldous QC relies upon the evidence of Mr Leach at paragraph 3.24 of his report where he stated:
- This issue was further addressed by the experts at the JEM. In answer to the Defendant's agenda asking the question:
- When he gave evidence, Mr Leach was cross-examined by Mr Havers QC about the additional risk, if any, of giving chemo-prophylaxis within six hours of surgery. Mr Leach was referred to the paper by Gerlach and others where, as stated earlier in this judgment, chemo-prophylaxis was given between 12 and 24 hours post-operatively. Mr Leach pointed to the limitations of the Gerlach paper:
- I cannot agree with Mr Havers QC in his suggestion that the starting point and the end point is Mr Leach's acceptance in his evidence that there is no evidence in the medical literature that giving chemical prophylaxis within six hours of spinal surgery increases the risk of post-operative haemorrhage. If that were right, then there would be no judgment of the risk/benefit balance to be made and no reason not to start chemo-prophylaxis very early in all cases, which is clearly not what NICE recommends in 2018 and, as I have found, was not the practise amongst spinal surgeons in the UK at the time. The only reason that NICE, reflecting current medical practise, recommends delaying the giving of chemo-prophylaxis routinely until 24 hours after surgery must be because of a perceived risk to the patient from giving it earlier. This makes medical sense. Surgery is a form of trauma and in lumbar surgery the muscles are stripped away from the bone in order for the laminectomy to be carried out. Some bleeding is inevitable, as Mr Tolias conceded, and therefore you expect to find "normal" blood clot formation at the site of surgery. However, it is to be hoped and expected that the blood will clot, the bleeding will stop and the body's normal defence mechanisms will take over. Clearly, an anti-coagulant will, by definition, interfere with those clotting factors and make both the chance of bleeding and the extent of bleeding greater. In re-examination, Mr Leach said:
- Finally, in terms of causation, it is necessary to consider whether the formation of the haematoma in terms of its size was causative of the neurological deficit to which Mrs Lesforis has been subjected. Clearly, what has happened in this case is unusual: it is difficult to understand why compression of the cord at the L 3/ 4 level should affect the L5/S1 nerve roots to devastating effect, but not the L3/4 nerve roots, nor the S2-4 nerve roots. Thus, although Mrs Lesforis suffered some weakness of the hips and knees, this was not outwith that which would be expected in a woman who had undergone major spinal surgery and had been nursed flat in the post-operative period. By the time Mr Al-Barazi saw Mrs Lesforis at 9am on 1 July 2013, her knee and hip movements were almost normal (4-5/5). Nor is it easy to understand why, if the L5/S1 nerve roots were "wiped out", the same should not have happened to the other sacral nerve roots contained within the dura at that point. However, the preservation of perianal sensation and the function of the anal sphincter indicates that the S2 S4 nerve roots were unaffected.
- In the end, though, this conundrum has been solved for me by Mr Cadoux-Hudson's agreement and concession in his report at paragraph 6D that, despite the unusual presentation, "overall haematoma formation was the more likely cause." He did not resile from this view in his oral evidence. Mr Cadoux-Hudson considered that the problems faced by Mrs Lesforis were consistent with a compressive haematoma. In cross-examination there was the following exchange:
- In his submissions, Mr Havers QC invited the court to find that, notwithstanding that Mr Cadoux-Hudson maintained his view that the more likely explanation was a compressive haematoma, on the totality of the evidence this is unlikely to have been the case. However, that is an invitation which I decline to accept. In the face of agreed expert evidence that compressive haematoma was causative of the injuries sustained in this case, it would be a bold judge who rejected that evidence and decided that he knew better than the experts on this medical issue. In the end, Mr Tolias noted in his dictated medical report that, when he re-operated, "just epidurally there was a clot of identified solidified [matter] and causing compression of the dura itself" and thus there was a compressive haematoma liable to cause damage. That evidence forms a solid foundation for the views of the two experts and, given the medical complications in this case, I could not possibly gainsay their view.
- It follows that, in relation to the first allegation, namely the inappropriately early prescription of chemo-prophylaxis, both breach of duty and causation are made out thereby entitling the Claimant to judgment.
- Given my finding in relation to the allegation of negligence in the timing of chemo-prophylaxis, I can take the issue relating to delay in re-operating relatively shortly. On behalf of the Claimant, it is alleged that Mr Tolias, not having been able to exclude a compressive haematoma as the cause of Mrs Lesforis' symptoms, should immediately have re-operated to explore the wound and to evacuate any haematoma. Although an MRI scan would have been a useful additional part of the diagnostic armoury, if no MRI was immediately available (as it was not), then Mr Tolias was obliged to re-operate as quickly as possible. It is the Claimant's case that, given that Mr Tolias found a compressive haematoma (in the sense that the haematoma was compressing the dura), he clearly cannot have excluded a compressive haematoma and therefore, on his own admission, should have re-operated as an emergency.
- For the Defendant, it is submitted that the position was not as simple as that. It is important to look at the situation as it appears to the Defendant at the time and not through the "retrospectoscope". Mr Tolias is an experienced and respected consultant neurosurgeon who gave his full attention to Mrs Lesforis as soon as he was aware of this problem. He arranged for her to be seen by Mr Al-Barazi straightaway, Mr Al-Barazi being on the premises, and he arranged for an emergency CT scan which was reported on by Dr Connor, a Neuroradiologist whom he knew and trusted. Dr Connor's evidence was that he spoke to Mr Tolias and relayed to him his interpretation of the CT scan. This showed that there was a compressive haematoma, but at the L1/2 level, not at L5/S1 which appeared to be the origin of Mrs Lesforis' neurological deficit. He said that although he couldn't exclude a compressive clot at L3/4 on 100% basis because of artefact on the CT scan, there was an "incredibly low probability" of haematoma at the site of the laminectomy. Given that, in his operation note, Mr Tolias says that there was "a clot of identified solidified [matter] and causing compression of the dura itself" the information being relayed to him by Dr Connor appears not to have been accurate but, as stated, it is necessary to look at the position from Mr Tolias' standpoint at the time. In that respect, the clinical position confronting him was puzzling and confusing. There was a sudden loss of ability by the Claimant to move her ankles and toes, indicating a motor problem at the L5/S1 level but there was no serious sensory loss in the form of cauda equina syndrome, with perineal sensation remaining intact. Although there was some weakness in the knees and hips, this was not very serious and was consistent with a woman who had been immobilised after serious spinal surgery. The development was surprising in the following respects:
- This course of conduct was one which Mr Tolias discussed with his colleagues who supported his plan. Those colleagues included Mr Malik, an experienced spinal surgeon.
- In addition to Maynard, Mr Havers QC also refers me to the decision of the Court of Appeal in Hughes v Waltham Forest Health Authority [1991] WL 839495. This claim arose out of the death of a patient who developed complications in association with a gallstone. It was alleged that there had been a failure to refer the deceased for endoscopic retrograde cholangio-pancreatocography ("ERCP"). At first instance, the judge had said:
- For the Claimant, Mr Aldous QC submits that the fact that Mr Tolias consulted with his colleagues is neutralised by his omission to give them one piece of vital clinical information, namely that, on examination, there had been found to be weakness of the hips and knees which was potentially indicative of a problem emanating from the level of the operation, namely L3/4. Although, in isolation, some weakness of the hips and knees would not be regarded as particularly sinister after spinal surgery of this kind in an obese woman who had been nursed flat for almost two days after the operation, the clinical information took on greater significance in the context of complete motor loss in the ankles and toes. Thus, Mr Aldous QC submits that, without being told this information, the endorsement of Mr Tolias' proposed course of action by Mr Malik, for example, loses its force. Mr Aldous QC submits that the simple question is whether Mr Tolias had excluded a compressive haematoma: if he had not, then he was obliged to re-operate. Mr Tolias did so at about midnight in circumstances where the clinical situation had not changed at all. He submits that this delay was illogical and once it is conceded that re-operation was appropriate, it should have happened immediately and not after a delay of some eight hours.
- In my judgment, although there are neurosurgeons who would have disagreed with Mr Tolias' strategy - and Mr Leach is one of them - it cannot be said that his decision making was so outwith usual practise as to have been negligent. He was faced with a very difficult clinical situation and he took a considered view. He could not exclude from that consideration the risks of further surgery, which are not negligible. Had he operated immediately and a complication of surgery occurred, he could have been criticised for "diving into" a re-operation rather than considering the position and waiting to see if it improved with treatment. As Mr Havers QC put it, this was a situation of "damned if you do, damned if you don't".
- In the circumstances, I find that there was no negligence on the part of Mr Tolias in relation to his decision-making on the afternoon and evening of 29 June 2013: indeed, he could have been criticised for re-operating in the face of the advice he was given by Dr Connor that the chance of a compressive haematoma at the site of the previous surgery was "incredibly low".
- Had I found negligence on the part of Mr Tolias in delaying his re-operation, causation would have been complicated. However, there would in my view have been some significant improvement in Mrs Lesforis' condition. Thus, her motor deficit had come on within the 12 hour period before surgery and, given the compressive component, relief from the compression could have been expected to allow the nerve roots a degree of recovery. However, recovery would not have been complete, and Mr Leach accepted in the JEM that there would in any event have been some long-term disturbance of bladder function and some neuropathic sensory symptoms, but these would have been less severe than with delayed surgery. Thus, I would have found that the quantification of the claim should proceed upon the causative basis proposed by Mr Leach. However, in the event, the problem does not arise because, without the formation of a compressive haematoma at all, Mrs Lesforis would have made a complete recovery and that is the basis upon which the case is to be quantified, given my findings in relation to the first issue.
- Finally, I shall say something about the pleaded allegation that Mr Tolias was negligent in failing to undertake emergency MRI investigation within 2-3 hours of the first complaint of adverse neurological symptoms. I have to express surprise that, in 2013, a consultant neurosurgeon was carrying out complex spinal surgery on a patient in circumstances where there were no out-of-hours emergency MRI facilities on site. However, this appears to have been the responsibility of the Harley Street Clinic, not the responsibility of Mr Tolias. It might have been alleged that Mr Tolias should have arranged for there to be an on-call radiographer available to carry out emergency MRI scanning should that be required, the Clinic having the equipment necessary on site and Dr Connor being available to review the MRI remotely. However, this was not alleged, nor was it alleged that Mrs Lesforis had been inadequately consented for the operation in so far as she consented to have an operation at a hospital where there were no facilities for emergency out of hours MRI scanning.
- Not only is it alleged that Mr Tolias failed to undertake emergency MRI investigation but also that he used "inadequate imaging (namely the CT scan of 29 June 2013 which failed to identify the compressive thrombus) as a basis for the treatment plan". As it turns out, in retrospect, it seems correct that the CT scan gave inadequate imaging because it failed to identify the compressive thrombus which Mr Tolias then found when he re-operated at midnight. However, it seems to me that both Mr Tolias and Dr Connor were led astray by the clinical situation which appeared to show a problem emanating from below (distal to) the site of operation, namely L5/S1. Dr Connor believed that he was able to advise Mr Tolias fully on the basis of the CT scan and Mr Tolias acted accordingly. In my judgment, it is likely that, had MRI scanning been available in an emergency, it would have been done as Mr Tolias would have wanted to have the full radiological picture, but in the circumstances in which he found himself, he acted reasonably in proceeding on the basis of the CT scan and the advice he was being given by Dr Connor.
- In the circumstances, there shall be judgment for the Claimant.
- Finally, may I pay tribute to the Claimant's solicitors for the way in which the trial bundles were prepared, and in particular for the reduction of the medical records to a core bundle in a single lever arch file: although the full medical records comprising 5 lever arch files were made available, it did not become necessary at any stage to go beyond the core bundle. This made the task of the court significantly easier, for which I am grateful.
Mr Justice Martin Spencer:
Introduction
History
The treatment by Mr Tolias
"We reviewed together the MRI scan from April of last year which revealed an L3/4 grade 1 spondylolisthesis with narrowing of the lumbar canal and exit foraminal stenosis. I demonstrated this to Mrs Lesforis and explained that this is the cause of her symptoms but obviously clinically she is improving and therefore intervention at this point is not warranted. I suggested that she continues with her efforts to lose weight and to also take up some exercise like swimming, walking, cycling which will improve her overall fitness and that will help with her pain as well.
With regards to surgical intervention in the spine, there is a likelihood that it might be necessary in the future as osteoarthritis progresses, however at the moment as her clinical symptoms have almost disappeared there is no reason to intervene. I will review her routinely in six months time and we can make plans either for discharge or surgery at that point."
"It is almost six months since her last review. Unfortunately her symptoms continue to be present, in particular on the left side and it does not seem that she is improving significantly. I explained that I am happy to offer her a lumbar decompression and postero-lateral fusion of the level in order to improve her pain in the back as well as her leg pain. She still wants to think about it. I described the procedure to her including the risks, including risks of damage to the nerve, CSF leak, infection, haemorrhage, failure to improve, recurrence of problems. She will think about it and let me know. In the meantime I have requested a repeat MRI and CT scan of her lumbar spine and we will let you know of her progress."
The MRI, carried out on 8 October 2012, was reported as showing a seven millimetre anterior subluxation of the L3 vertebral body upon L4 causing moderate to severe canal stenosis and bi-lateral moderate foraminal stenosis with some impingement of the exiting nerve roots. These appearances were similar to those from April 2011.
"I described the procedure once more. I explained the risks including the risk of leg weakness, paralysis, loss of bowel and bladder control, persistent pain, haemorrhoids, infection, failure to improve DVT or numbness. In view however of the persistent problems the benefits outweigh the risks. Mrs Lesforis is keen to proceed, I gave her a booklet to read and she has signed the consent form."
The consent form, also dated 20 February 2013 and signed by Mrs Lesforis, contained the following:
"I have explained the serious or frequently occurring risks and risks of particular significance in the patient's circumstances. If patients make clear they have particular concerns about certain kinds of risk, discussion must include information about these risks, even if they are very rare and those discussions must be documented here. I have stated that any additional procedures at the time of operation will only be performed to protect the patient's life or future well-being.
Leg weakness/paralysis/loss of bowel/bladder/ CSF leak/persistent pain/haemorrhage/infection/failure to improve/DVT/numbness."
Thus, it seems clear that the Claimant was comprehensively warned of the risks of surgery which she was electing to undergo and Mrs Lesforis does not assert otherwise.
The deterioration
"Patient complained of not feeling her legs. There was minimal WB. Unable to wiggle toes once in bed.
Plan: discuss with Mr Tolias.
[Telephone conversation] with Mr Tolias, explained patient can't feel her legs, and was unable to wiggle toes in bed."
"Says that today she had difficulty walking
Can feel her legs well, ? less so on left; can feel catheter tug
o/e: normal sensation to soft touch L3 S1
No ankle movements, unable to wiggle toes
Hip flexion 3/5 B ext. 4/5
Knee flexion 3-4/5 B ext. 4/5."
Mr Al-Barazi noted that Mrs Lesforis was to have a CT scan of her lumbar sacral spine and that he would then discuss the case with Mr Tolias.
" an MRI scan was not possible at the Harley Street Clinic out of hours or on the weekends. No MRI trained radiographers were on call at HSC or at the nearby private hospital. If a clinical emergency necessitated an MRI scan then the patient would, most likely, have been transferred to an NHS emergency department. I do not know how long this would have taken but it might well have been several hours."
Mr Tolias also suggests in his witness statement that a CT scan was preferable to MRI, stating:
"The difficulty with MRI as an alternative modality in these circumstances is multi factorial. In the first place, post-operative MRI is not very good at showing acute blood and blood products. The interpretation is even more difficult when metalwork is present. The next problem was that we had put titanium in her spine and whilst this is not sensitive to a magnet, it does create signal change, an artefact which makes it harder to interpret an MRI. Above all, there was no problem with the imaging of the area of the spine about which we were concerned: the CT scan showed that there was no lesion in her lower spine the area distal to where we had operated and where her symptoms pointed to a problem. It was vanishingly unlikely that MRI would have provided more information about that area."
In my view, this passage smacks of retrospective justification for a failure which, in reality, Mr Tolias recognised, which is that, in 2013, any surgeon carrying out spinal surgery of this kind needs to have arrangements in place for emergency MRI scanning. It may be true that, in terms of visualising the metalwork, CT scan gives as good a view as MRI, but that is not true of visualisation of soft tissue and nerve roots. I shall return to this issue in paragraph 75 below.
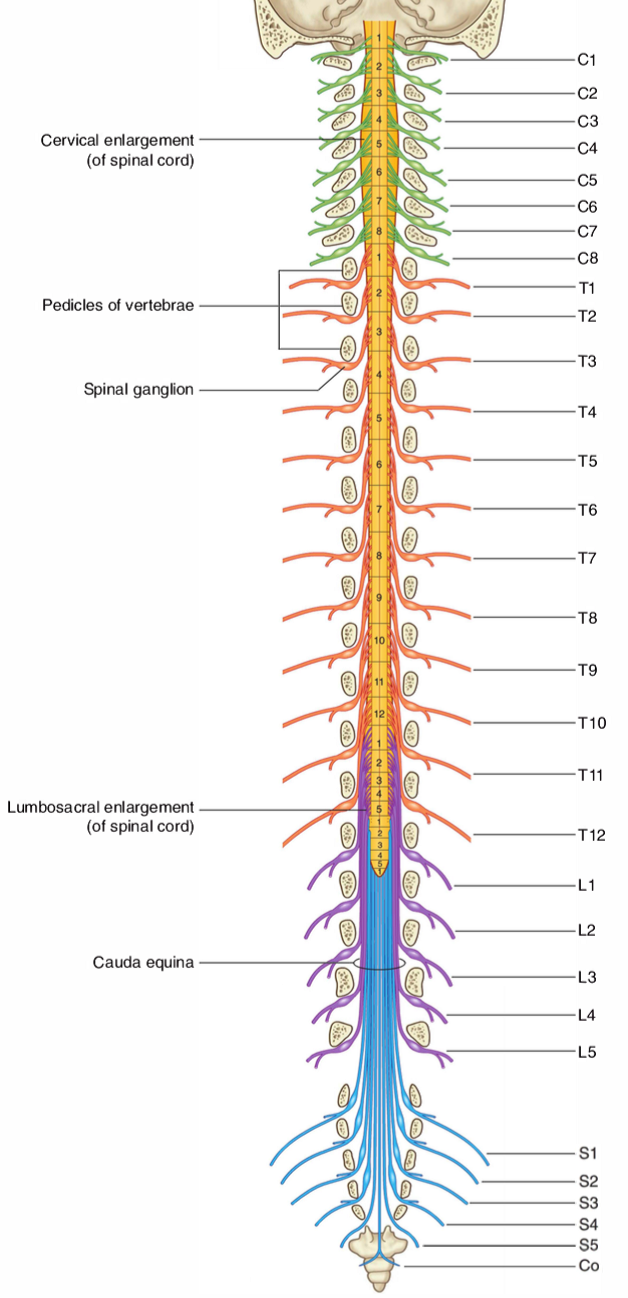
As seen, the nerves, controlling different functions, exit the spinal column at different levels. Damage to the spinal cord will affect the nerves which remain in the cord at that level, but not those which have already exited at a higher level. Thus, clinically, the presentation of a patient may give the surgeon a strong clue as to the likely level of any lesion or problem affecting the spinal cord. In the course of the evidence, Mr Leach, the Claimant's neurosurgical expert, produced a document from the American Spinal Injury Association ("ASIA") showing International Standards for Neurological Classification of Spinal Cord Injury. In terms of motor function, the chart shows the following key muscles affected by the nerves exiting at the following levels:
| L2 | Hip flexors |
| L3 L4 |
Knee extensors Ankle dorsiflexors |
| L5 | Long toe extensors |
| S1 | Ankle plantar flexors |
In terms of sensory function, the surface of the skin is divided into specific areas called dermatomes, a dermatome being an area of skin in which sensory nerves derive from a single spinal nerve root. Thus, a doctor can test for nerve root damage using a pin and testing for pin prick sensation. The key sensory points appear from the chart to be as follows:
| L1 | The hip girdle and the groin/inguinal area |
| L2 | Anterior aspect of each thigh |
| L3 | Anterior aspect of each thigh; anterolateral thigh and continues down to the medial aspect of the knee and the medial aspect of the posterior lower leg |
| L4 | Posterolateral thigh and the anterior tibial area |
| L5 | Posterolateral thigh wrapping around to lateral aspect of the anterior lower leg and dorsum of the foot; |
| S1 | Hips and groin |
| S2 | Back of the thighs |
| S3 | Medial buttock area |
| S4 | Perineal area |
| S5 | Perineal area |
"In conclusion, there are post-operative appearances as described following L3-4 laminectomy and pedicle screw and rod fixation. The intra-spinal ridges at site of surgery are markedly degraded by artefact from the pedicle screws. It is difficult to exclude some encroachment from dorsal epidural soft tissue swelling at the site of surgery. There is some equivocal intra-spinal soft tissue density extending superiorly within the upper lumbar canal. There is a locule of intrathecal air (? Related to intra-operative CSF leak) at L1 level. If further clarification of the imaging findings is required then MRI is suggested."
"I had excluded compression below the L4 level."
In relation to the area of the operative site he said that the impression on CT was of a slight bulge which is seen not infrequently in the post-operative situation but he accepted that a compressive haematoma could not be 100% excluded because of artefact at that level. However, he said that there was an incredibly low probability of compressive haematoma at the site of the laminectomy. Finally, Dr Connor said that there was an unusual finding at the L2 level which he could not explain but which appeared to be clinically irrelevant because, as stated, the origin of Mrs Lesforis' problems appeared to be much lower down at L5/S1.
"16.00 Tolias apparently patient very well until late last night
CT spine / d/w Steve Connor (consultant neuroradiologist) ? no obvious acute clot
"The clinical and radiological picture did not suggest an acute, clinically significant compressive haematoma, that neuropraxia was more likely and the best thing was to give steroids to reduce the potential oedema and to observe her closely, but to re-operate if she did not improve within a few hours."
"Mr Tolias came to review the result of the scan. Plan is for her to start on steroids ASAP and also to sit out. Continue on physio input and neuro obs. If pt not improved by Monday: then MRI scan. Dexamethasone 4 mg given."
It has to be said that the plan disclosed by the nursing notes does not appear to be consistent with the plan which Mr Tolias said was the actual plan, namely to re-operate if Mrs Lesforis did not improve within a few hours. Mr Aldous QC submits that the nursing note genuinely represents Mr Tolias' plan at that stage, and betrays his muddled and illogical thinking at that time. Mr Havers QC submits that, given the subsequent events, it appears that the nurse may have mis-understood what Mr Tolias was saying, or alternatively that Mr Tolias' plan was relayed to her through a second or third party and became garbled in the process.
"Mrs Lesforis was improving well following her procedure and was moved on to the ward after her stay in the Intensive Care Unit. However, unfortunately on the morning of 29 June, she quite suddenly noticed that she could not really move both her feet. She did not experience any significant pain or any other symptoms but she reported that some time during the night she felt something happening in her legs. When the physiotherapist tried to mobilise her on Saturday morning, it proved impossible. She was reviewed immediately by my colleague, Mr Barazi, who was in theatre at Harley Street, and he noticed that there was complete weakness of the plantar and dorsiflexion of both feet (0/5), 4/5 on knees and 4/5 on hips. There was some sensory hypoaesthesia in the S1 dermatome. Mrs Lesforis could feel her bladder catheter tug. There was anal wink and was, on inspection, ability to squeeze her anal sphincter. An emergency scan of the lumbar spine was organised which was reviewed by our neuroradiology colleague, Dr Steve Connor, and there was some retrodural collection which we expected in view of the patch that we created to protect her from the CSF leak. There was no real evidence of a large clot, both above and below the decompression area. The screws were in good positions. The left upper screw at L3 was slightly more medial but there was no other evidence of problem. We started Mrs Lesforis on a course of steroids but over the next few hours no specific improvement was noticed in her feet. She was still quite briskly lifting both her legs off the bed but was unable to move her feet. In view of that and due to lack of any improvement, we decided to proceed to exploration of the wound in order to at least exclude the possibility of a significant compression of the nerve rootlets and theca by any clot."
"After general anaesthetic she was given a further dose of antibiotics, positioned prone on a Montreal mattress, and the wound was re-opened. Copious amounts of Betadine saline were instilled. There were no clots in the superficial layers however just epidurally there was a clot of identified solidified [matter] and causing compression of the dura itself, which was removed with copious amounts of wash and pituitary rongeurs. It was found that the epidural veins, particularly in the anterior aspect of the laminectomy, were oozing continuously and it took considerable effort to stem the bleeding using Flowseal pressure and wash. Again the wound was washed with Betadine saline and closed in layers with staples to skin over Redivac drain and suction this time."
"Tolias
No significant change
Still 0/5 at the ankles, 3/5 knee extension/4/5
Able to lift leg off the bed
Can feel catheter/anal tone present unable to squeeze
100 ml in drain
[Treatment]
Remove drain
Can mobilise
Will need intense physio and rehabilitation."
This note is supplemented by the final part of Mr Tolias' dictated medical report of 1 July 2013 where he states:
"Post-operatively Mrs Lesforis recovered well from the procedure. She noticed some subjective improvement, in particular in the sensation in her legs but the next morning she could still lift her legs off the bed but could not move her feet still. On examination she could feel the catheter and there was anal tone but she could not squeeze on the finger. We agreed that she will try to mobilise. I explained the seriousness of the situation and I also contacted her husband about it. We agreed with the physiotherapist that we will continue to mobilise as able, remove the drain at 24 hours and assess neurological improvement. Following this, I contacted Mrs Lesforis' GP, Dr O'Leary in order to try to arrange some neuro rehabilitation support for her as it is obvious that she will require more long term support until she is stabilised or further improves."
"DW [discussed with] Mr Tolias, happy for patient to be mobilised gently this morning. Patient went to theatre last night, due to blood clot." (emphasis added)
The rest of the physiotherapist's note is not relevant for present purposes.
"Op note findings noted
Patient feels 'Better in myself'
Hip + knee movements 4-5/5 (bi-lat)
No ankle movements; no toe movements
Feels catheter tug
Normal sensation to soft touch
Feet warm and well perfused"
The plan was for her to continue with physiotherapy.
The allegations against the Defendant
a) Whether it was negligent to administer Clexane (that is, chemo-prophylaxis in the form of LMWH) within six hours of the operation;
b) [Diagram or picture not reproduced in HTML version - see original .rtf file to view diagram or picture]Whether it was negligent to delay intervention after 14.30 until surgery at midnight;
c) Whether the early administration of Clexane and/or the delay in intervention were causative of the permanent nerve damage that reduced the Claimant's mobility and left her using a wheelchair.
I agree that these are the principal issues for determination in this case, although I also need to say something about the pleaded allegations of negligence in relation to the failure to carry out MRI scanning. I shall deal with causation in conjunction with the allegations of breach of duty rather than as a separate third issue.
Issue 1: Was it negligent for the Defendant to arrange for the administration of chemo-prophylaxis within six hours of the operation?
"13. At the end of the operation I prescribed subcutaneous Clexane for her once daily. I see that that prescription is criticised and I can only say that it is my invariable routine to give patients anti-coagulation after this sort of operation. An overweight patient such as Mrs Lesforis, particularly one who is going to remain flat for 48 hours after the operation because of the durotomy, is at increased risk of venous thromboembolic events and therefore Clexane is indicated, along with intermittent calf compresses which were also prescribed (in accordance with NICE guidelines). However, it is my normal practice to give anti-DVT chemo-prophylaxis (Clexane) very early post-operatively to all my cranial or spinal patients and I am surprised to see it is criticised in the Letter of Claim."
Of course, the giving of chemo-prophylaxis is not criticised as such, rather it is the timing which is criticised. From Mr Tolias' statement, it seems clear that, in relation to the timing, he did not discriminate between his patients in this regard: thus, he did not say that he prescribed Clexane that early post-operatively for Mrs Lesforis because of any particular individual circumstances pertaining to her particular case. Rather, he said that this is the timing for all his cranial and spinal patients.
"3.3 as a Posterior Lumbar Inter-body Fusion can be associated with a post-operative haematoma compressing the thecal sac and this can cause cauda equina syndrome, chemo-prophylaxis against venous thromboembolism is not given in the very early post-operative period. Mechanical prophylaxis in the form of graduated compression stockings and Flowtron boots are used in the first 1224 hours post-operatively. Chemo-prophylaxis against venous thromboembolism is usually commenced on the first post-operative day. The commencement of chemo-prophylaxis against venous thromboembolism within six hours of surgery increases the risk of post-operative haematoma formation."
Although Mr Leach acknowledges that the surgeon must exercise judgment when deciding on appropriate timing of chemo-prophylaxis he states that to prescribe it within six hours of a Posterior Lumbar Inter-body Fusion represents a breach of duty. He states:
"3.12 a reasonable spinal surgeon would exercise caution with the use of post-operative chemo-prophylaxis against venous thromboembolism. This is because chemo-prophylaxis against venous thromboembolism increases the risk of a post-operative haematoma. That risk of haematoma formation decreases with time, such that use of chemo-prophylaxis 12-24 hours post-operatively has a much lower risk of association with post-operative haematoma than administration of the same drug within six hours of surgery.
Although the NICE guidelines are silent on the issue of timing of chemo-prophylaxis following major spinal surgery, my clinical experience informs me that it would be normal to commence chemo-prophylaxis the day after surgery, such as a Posterior Lumbar Inter-body Fusion and you use mechanical prophylaxis in the form of graduated compression stockings and compressive Flowtron boots in the first 24 hours. In my opinion, it represents a breach of duty to prescribe a medication associated with increased risk of post-operative haematoma formation within six hours of the completion of a Posterior Lumbar Inter-body Fusion."
"The use of Low Molecular Weight Heparin (LMWH) (subcutaneous slow release or IV) has been variably introduced across the UK. Some neurosurgical and spinal units give a LMWH type medication, (anti-coagulant) routinely 12-24 hours after spinal surgery unless the operating surgeon specifically states otherwise. my own practice in this situation is to prescribe LMWH at 24 hours after this type of surgery usually an hour or so after the wound drain has been removed."
This was hardly a ringing endorsement of Mr Tolias' routine practice to give very early chemo-prophylaxis: indeed, Mr Cadoux-Hudson did not suggest that there was a reasonable body of spinal surgeons in the UK in 2013 who would give chemo-prophylaxis at such an early stage as opposed to 12-24 hours after spinal surgery.
"Was it appropriate to prescribe chemo-prophylaxis against venous thromboembolism within six hours of surgery?"
The experts provided the following answer:
"The experts agree that there is paucity of good quality clinical evidence on the subject of timing of chemo-prophylaxis against VTE following spinal surgery. The NICE guidelines are acknowledged.
Mr Cadoux-Hudson notes that there are a number of different practices within surgery and particularly within neurosurgery. Whilst NICE guidelines exist for other surgical disciplines such as orthopaedics where venous thromboembolic prophylaxis is given before hip and knee surgery, neurosurgery units in 2012 had a range of times for extra dural spinal surgery ranging from before and after surgery.
Mr Leach holds the view there is not a reasonable body of spinal surgeons that administers chemo-prophylaxis against VTE within six hours of surgery.
NICE guidelines indicate a requirement to exercise a balanced judgment between risks of bleeding and risks of VTE. For procedures where post-operative bleeding can have devastating consequences, such as spinal surgery, mechanical prophylaxis is used in the peri-operative and early post-operative period and chemo-prophylaxis, if indicated, is delayed until the next day. Mr Leach notes that in neurosurgery there is some evidence of a bleeding rate of 2%."
"2 The Timing of chemoprophylaxis on 27th June 2013
2.1 Do you agree that there is a wide range of opinions about the optimal time to start chemoprophylaxis for Venous Thrombo Embolus (VTE)?
The Experts agree as this will depend on patient risk factors and type of surgery performed.
2.2 Do you agree that some surgeons start chemoprophylaxis for VTE:
a. before surgery?
b. some shortly after ?
c. some after 12 hours?
d. some after 24 hours?
e. some not at all?
The Experts agree. The timing of prophylaxis will depend on patient risk factors for VTE and bleeding risk of surgery.
2.3 Do you agree that there is little high level (Level One or Two) evidence covering chemoprophylaxis in patients undergoing cranial surgery and less in spinal surgery that supports any of these positions?
The experts agree.
2.4 Do you agree that the risks of fatal VTE are much greater than the risk of paralysis due to epidural haematoma as a result of chemoprophylaxis?
The experts partially agree.
The experts agree that the risk of fatal pulmonary embolism after extra-dural spinal surgery is rare, as low as 1:2000 whilst the rate of deep venous thrombosis as detected by ultra-sound is between 2-9%.
The experts also agree that the rate of epidural haematoma is also low (0.2-0.4%).
Mr Cadoux-Hudson states that the rate of epidural haematoma is not increased if early (before 24hrs) LMWT heparin is given (see Gerlach et al 2003).
Mr Leach states that the rate of paralysis due to epidural haematoma as a result of chemoprophylaxis is not known and that the NICE guidelines on VTE prophylaxis recognise this.
The NICE guidelines list lumbar puncture within the next 12 hours as a bleeding risk to be considered when deciding on the use of chemoprophylaxis against VTE. In this context, Mr Leach states that a Posterior Lumbar Interbody Fusion certainly represent a bleeding risk. The NICE guidelines state: "In spinal surgery the catastrophic long term neurological consequences of extradural bleeding need to be balanced against the risk to life of VTE disease."
Mr Cadoux-Hudson notes that lumbar puncture is an intra-dural procedure exposing intra-dural arteries and venous to direct trauma of the lumbar puncture needle, out of sight of the person performing the procedure and is not a reasonable analogy, for operative or post-operative Lumbar surgery.
2.5 Do you agree that Mrs Lesforis was at increased risk of VTE because:
2.5.1 She was slightly overweight:
The experts agree.
2.5.2 She was expected to be nursed flat for an extended period as a result of having sustained an intraoperative durotomy?
The experts agree.
2.6 Do you agree that there are some spinal surgeons who would have prescribed chemoprophylaxis against venous thromboembolism within 6 hours of surgery?
The experts disagree.
Mr Cadoux-Hudson, as pointed out above, is of the view that chemoprophylaxis is theoretically more effective the closer to the surgery event (best results have been demonstrated if given before surgery). The precise timing is at the surgeon's discretion, weighting the risks and benefits to the patient.
Mr Leach believes that there is not a reasonable body of spinal surgeons that would commence chemoprophylaxis against VTE within 6 hours of major spinal surgery.
2.7 Do you think that it can be said that their opinion does not stand up to analysis because there is sufficient evidence to show that it is dangerous?
The experts partially agree.
Mr Cadoux-Hudson sites Gerlach et al where LMWT heparin was given at 08.00hrs in the morning after surgery (within 24hrs) in over 1,299 patients undergoing lumbar surgery and no increase in the epidural haematoma rate or timing, with the largest group (5 of 13) developing the haematoma on the day of surgery (before LMWT heparin was given.
Mr Leach states that in the Gerlach study "early" is defined as prophylaxis commencing at 8am the day after surgery. None of the patients in this study had chemoprophylaxis commencing within 6 hours of surgery.
2.8 If so, can you identify the evidence?
Both experts agree that the evidence is limited.
Mr Cadoux-Hudson is of the view that the hypothesis was reasonably tested in the Gerlach et al paper and that some of the patients would have had LMWT heparin with hours of their operation.
Mr Leach states that the evidence does not support safe use of chemoprophylaxis within 6 hours of surgery and an element of judgement must be exercised as recognised in the NICE guidelines. Mr Leach does not believe that there is a reasonable body of spinal surgeons that commence chemoprophylaxis against VTE within 6 hours of major spinal surgery."
"Our study provides an up to date evaluation of the literature from across the world of the general estimate of the risks and benefits of using chemo-prophylaxis in patients undergoing cranial or spinal procedures. We found, based on moderate to good quality of evidence trials, that chemo-prophylaxis is beneficial in preventing VTE while resulting in no statistically significant increase in bleeding complications (both minor and major).
Conclusions
Based on the moderate to good quality of evidence, chemo-prophylaxis is beneficial in preventing VTEs in patients undergoing management of cranial or spinal pathology, with no significant increase of either major or minor bleeding complications. The adverse impact of VTE in untreated patients appears to outweigh that of haemorrhage in patients receiving chemo-prophylaxis. Further research is needed to determine whether this conclusion holds true for the more specific sub-populations, and for the optimal timing for initiation of chemo-prophylaxis."
Based on this passage, Mr Havers suggested to Mr Leach that the giving of chemo-prophylaxis does not give rise to any statistically increased risk of bleeding complications. Mr Leach disagreed with that proposition. He pointed out that the Khan paper, being a meta-analysis, provides no new research evidence that is not already in the literature and furthermore the study refers to the use of chemo-prophylaxis in a general neurosurgical population, but the authors were cautious not to apply their findings to particular patients such as those undergoing spinal surgery or Posterior Lumbar Inter-body Fusion. Mr Leach said that, looking at the detail of the Khan review, the only papers which looked at studies involving spinal patients which were reviewed were those by Gruber and Hamidi. He said that the conclusion drawn by the authors of the Khan paper were not borne out by the evidence from the papers which are pertinent to the present case.
"1.5.22 If using LMWH for people undergoing elective surgery, start giving it 24 - 48 hours post-operatively according to clinical judgement, taking into account patient characteristics and surgical procedure. Continue for 30 days or until the person is mobile or discharged, whichever is sooner.
1.5.23 If needed start LMWH earlier than 24 hours after the operation for people undergoing elective spinal surgery. Base the decision on multi-disciplinary or senior opinion, or a locally agreed protocol."
Mr Leach said that these guidelines very carefully reflect the evidence available at the time they were drawn up and NICE had come up with a conclusion that, if indicated, LMWH should be given at 24 - 48 hours post-surgery. He said:
"They are a long, long way from suggesting that chemo-prophylaxis is safe and it doesn't matter when you give it."
Although these NICE guidelines were not published at the time of the surgery to Mrs Lesforis, they do, to a certain extent, provide an answer to the suggestion that, as at December 2017 (the date of the publication of the Khan paper), the conclusion of those authors reflected the medical literature at that time.
"I had to look at the guidelines as they were at the time and look at the evidence and come up with an answer for the court about whether there was a reasonable body of surgeons in the UK spinal surgeons who gave early, less than six hours chemo-prophylaxis. It is a treatment that has a potential to cause significant harm, so there would need to be evidence of safety to do it. And on that basis my view is that there is not a reasonable body of surgeons who give chemo-prophylaxis very early after spinal surgery within six hours, because of the risk of haemorrhage. I'm not aware of a reasonable body of surgeons in the UK who give it pre-operatively and if I'm presented with evidence, for example that there is a protocol at King's College Hospital that all surgeons give it early or I'm presented with evidence that there is a body of surgeons that gives it early, within six hours, then I will accept that is reasonable. But where there is a lack of good clinical evidence and where there are just guidelines I do have to fall back and rely upon experience, having worked in many centres in the UK. I also noted Mr Cadoux-Hudson's statement that he also gives it in a delayed fashion, and I have not been presented within this process of any protocol or suggestion that there is a group of surgeons in the UK that give it within six hours. I will be prepared to alter that opinion if I was presented with evidence to the contrary."
i) The quality of the evidence is weak in that paper;
ii) The study did not compare giving chemo-prophylaxis early to giving it later;
iii) The study had 13 instances of haemorrhage which was treated immediately;
iv) 38% of the haemorrhages presented on day 2 or 3;
v) The implication from the paper is that none of the patients had prophylaxis within six hours.
"Unless the surgeon states otherwise. So we are back to this issue of protocol versus senior surgeon decision."
Mr Aldous interpreted this answer as meaning that the only case of which Mr Cadoux-Hudson would be aware of a reasonable body of practitioners administering LMWH within, say, three hours of surgery is if the surgeon specifically states that such early chemo-prophylaxis is necessary in the particular case. He then said:
"Well, my opinion is based on the evidence here that there is no strong guiding evidence either way. It is difficult for me to argue on a Bolam basis that this was below Bolam standards is what I think I'm trying to drive at. There is enough variation here to account for that, there is no specific data to say that three hours has a significantly higher risk than any other period."
"In 2013, with a patient who was overweight and who it was intended would spend the next 48 hours lying flat, would giving chemo-prophylaxis three hours post-surgery have fallen within the variation of practice in the UK which you referred to earlier in your evidence?"
To which Mr Cadoux-Hudson answered:
"Yes it would. Yes. "
He also agreed with the proposition that if a surgeon took the view that a patient who is overweight and would be lying flat for the next 48 hours should have chemo-prophylaxis three hours following surgery that would be a reasonable view for the surgeon to take. In answer to a question from the court, Mr Cadoux-Hudson said that there were surgeons in 2013 who had a system of giving LMWH on the evening of their surgery even if the surgery ended in the afternoon.
i) In 2013 there was no consensus among spinal surgeons as to when chemo-prophylaxis should be given in terms of timing post-operatively but there was a disparate range of practice;
ii) Mr Cadoux-Hudson said that he was aware of surgeons who have given chemo-prophylaxis within six hours;
iii) The NICE guidelines current at the time of this operation were silent as to the timing of chemo-prophylaxis;
iv) The Claimant had specific risk factors for VTE;
v) Mr Cadoux-Hudson stated that to give chemo-prophylaxis to such a patient three hours following spinal surgery in the UK in 2013 would have fallen within the variation of practice to which he referred;
vi) Mr Cadoux-Hudson said that if a surgeon had taken the view that it was appropriate to give chemo-prophylaxis three hours following spinal surgery then that would have been a reasonable view for the surgeon to take given the variation in practice;
vii) It was Mr Cadoux-Hudson's view that it is reasonable to give it within six hours;
viii) There is no evidence in the medical literature that giving chemo-prophylaxis within six hours increases the risk of post-operative haemorrhage.
"We are dealing with a situation here where a senior neurosurgeon, an experienced neurosurgeon, has taken into account the risk factors before him at the end of the operation with another neurosurgeon who is operating with him, Mr Malik, and a consultant anaesthetist, and typically in my experience these discussions are things that you start discussing during the procedure, and I suspect it would have happened during the procedure because one of the decisions that was made was made on the basis of the incidental durotomy. So a fairly significant amount of thinking has gone on, if that is the right way of putting it, to consider the use of Low Molecular Weight Heparinoids."
In response to this Mr Aldous QC suggested that Mr Cadoux-Hudson was assuming such a discussion took place because it should have, to which Mr Cadoux-Hudson responded:
"Because it can do. In the guidelines it is about senior surgeons making that decision."
Mr Aldous QC was critical of Mr Cadoux-Hudson because he was speculating about a matter which was not in fact reflected in the evidence of either Mr Tolias or Mr Malik.
"Had [Mr Tolias] carried out a proper risk assessment then he has not said what conclusion he would have come to. On the evidence it is likely that he would or should have come to a similar conclusion to that of the only two witnesses to have addressed the issue, the experts, who would have waited. Thus the bleeding and its consequences would have been avoided."
"I am not saying that there weren't any surgeons around the world who had studied pre-operative chemoprophylaxis. I had to look at the guidelines as they were at the time and look at the evidence and come up with an answer for the court about whether there was a reasonable body of surgeons in the UK spinal surgeons who gave early, less than 6 hours chemoprophylaxis. It is a treatment that has a potential to cause significant harm, so there would need to be evidence of safety to do it. And on that basis my view is there is not a reasonable body of surgeons that give chemoprophylaxis very early after spinal surgery, within 6 hours, because of the risk of haemorrhage."
Discussion
"Was it appropriate to prescribe chemo-prophylaxis against venous thromboembolism within six hours of surgery?"
Mr Cadoux-Hudson responded:
"Mr Cadoux-Hudson notes that there are a number of different practices within surgery and particularly within neurosurgery. Whilst NICE guidelines for other surgical disciplines such as orthopaedics where venous thromboembolic prophylaxis is given before hip and knee surgery, neurosurgery units in 2012 had a range of times for extradural spinal surgery ranging from before and after surgery."
It seems to me that if Mr Cadoux-Hudson was aware of other neurosurgical units who routinely administered LMWH within six hours of spinal surgery, this was the moment when he could and should have said so. Had he done so, I am sure that Mr Leach would have conceded the point. However, he did not and it seems to me likely that this is because he was not so aware. Question 2.6 of the Defendant's agenda asks the question:
"Do you agree that there are some spinal surgeons who would have prescribed chemoprophylaxis against venous thromboembolism within six hours of surgery?"
To this Mr Cadoux-Hudson responded:
"Mr Cadoux-Hudson, as pointed out above, is of the view that chemo-prophylaxis is theoretically more effective the closer to the surgery event (best results have been demonstrated if given before surgery). The precise timing is at the surgeon's discretion, weighting the risks and benefits to the patient."
It seems to me this is not an answer to the question and Mr Cadoux-Hudson's failure to answer the question directly is surprising.
"It represents a breach of duty to prescribe chemo-prophylaxis against venous thromboembolism within six hours of a Posterior Lumbar Inter-body Fusion".
Dealing with the arguments raised by Mr Havers QC:
i) Although I accept that there was quite a disparate range of practise across the UK in relation to the timing of the giving of chemo-prophylaxis after spinal surgery, in my judgment this range will have been within the period 24 hours to 48 hours post-surgery or perhaps 12 hours to 48 hours post-surgery but not within six hours of surgery. Thus, whilst I accept that there was no consensus amongst spinal surgeons in the UK in 2013 as to when chemo-prophylaxis should be given in terms of timing post-operatively, I do not accept that there was no such consensus as to when chemo-prophylaxis should not be given. I accept Mr Leach's evidence that no reasonable body of spinal surgeons in 2013 would have given chemo-prophylaxis routinely within six hours of spinal surgery in 2013. To give such early chemo-prophylaxis required specific justification in the specific circumstances of the case having weighed the risks and benefits of so doing.
ii) Although Mr Cadoux-Hudson stated that he was aware of surgeons who gave chemo-prophylaxis within six hours, I do not accept that evidence: had he been so aware, I consider he would have said so much earlier than re-examination, probably in his report and certainly in the course of his discussion at the JEM with Mr Leach.
iii) It is true that the guidelines current in 2013 said nothing about the timing of giving of chemo-prophylaxis after spinal surgery. The 2018 guidelines do and suggest that, for routine chemo-prophylaxis, the appropriate time period is 24 48 hours after surgery (which accords with the practise of both Mr Leach and Mr Cadoux-Hudson). These guidelines are likely to reflect the practise that was common in the UK in the year or so before their publication, that is in 2016/2017. In my judgment, it is extremely unlikely that practise in the UK in 2013 was significantly different. If anything, the movement after 2013 was towards giving chemo-prophylaxis to more patients and sooner, that is a liberalisation of practise in the UK, and for these reasons the 2018 NICE guidelines are of some help.
iv) I accept that there were three risks factors for VTE in the Claimant's specific case, namely that she was overweight, she was expected to be immobile for 48 hours post-operatively and that her anaesthetic and surgery time had exceeded 90 minutes. However, these were reasons for giving the Claimant post-operative chemo-prophylaxis against VTE: they do not speak to the timing of the prophylaxis.
v) In so far as Mr Cadoux-Hudson stated that, in his view, the giving of chemo-prophylaxis to a patient such as the Claimant within three hours would have fallen within the variation in practise to which he referred and would have been reasonable, I do not accept that evidence but I prefer the evidence of Mr Leach in that regard.
Causation
"The complexity in this case one of many - is that the symptoms developed on the Saturday, the 29th, by which time she had received two doses. So now the issue is how much of the first dose would still be active in the early hours of the Saturday? And the evidence is that when Clexane is given, it reaches its peak effect in the blood stream four hours after you give it and then it has a half-life of around four hours, so every four hours that follows the concentration and its effect fall. It is removed by the kidneys. So therefore the activity of Clexane by 8 o'clock from the first dose the following day would be negligible or very small, hence the need to give another dose. And so therefore, had she not received the dose on the evening of the operation, but had merely received her dose on the Friday, 24 hours after the surgery, she was still at risk of a haematoma the following morning."
In answer to a question from the court "Are you assuming the haematoma occurred at about the same time as the symptoms?" Mr Cadoux-Hudson replied:
"I'm assuming that it may have preceded by a few hours but that sort of period of time. These haematomas are often complex and they may have a number of components to them, but I think the answer to the symptoms gives us some idea as to the temporal relationship to the clot forming."
"But for the breach of duty in prescribing and administering Enoxaparin chemo-prophylaxis against venous thromboembolism within a few hours of a Posterior Lumbar Inter-body Fusion, Mrs Lesforis would, in all probability, have avoided the complication of post-operative epidural lumbar haematoma and would not have suffered a neurological deficit as a result of the surgery."
"Do you consider the Enoxaparin to have caused, or materially contributed to, the development of the [haematoma], on the balance of probabilities?"
To this they responded:
"Mr Cadoux-Hudson recognises that LMWT Heparin such as Enoxaparin is an anti-coagulant and therefore theoretically can alter systemic blood clotting. However, a large study (more than 1,000 lumbar spine operations, LMWT Heparin given within 24 hours) failed to demonstrate an increased risk of epidural haematoma, with more than a third of epidural haematomas occurring before the Heparin was given to the patient. This observation suggests that Enoxaparin at the dose given would not have altered the systemic blood clotting capacity to alter wound haematoma formation.
Mr Leach is of the opinion that LMWT Heparin, such as Enoxaparin, should not be given within six hours of major spinal surgery due to the risks of bleeding that could cause a catastrophic neurological outcome."
"As they state, this is a retrospective series with no case control, so the level of evidence is weak. They were not comparing early use of Heparin against later use; they are just describing having a retrospective case series. They did have 13 instances of post-operative epidural haematoma in this series, 13 patients. They treated all of them immediately immediate treatment and with immediate treatment, 60% of the patients experienced a full neurological recovery. They also comment that 38% of the haematomas presented at day 2 and 3. So although they commonly present straight away, 38% present late. So there are a number of different conclusions from the paper. The headline one, I would say, is that this is weak evidence that use of chemo-prophylaxis at between 12 24 hours in this series didn't show a higher rate of epidural haematoma than other reported case studies. That is how I would conclude an assessment of this paper."
Mr Havers QC asked Mr Leach whether there is any evidence in the medical literature to say that giving chemo-prophylaxis before 24 hours increases the risk of post-operative haemorrhage. Excluding the Gruber paper where the Heparin was given pre-operatively, Mr Leach confirmed that there was not, because it had not been well studied:
"A: It has not been well studied, giving chemo-prophylaxis within six hours. Within six hours has not been studied.
Q: So the answer to my question is that there is no evidence in the medical literature that giving chemical prophylaxis within six hours of spinal injury increases the risk of post-operative haemorrhage?
A: I agree. And the experts have agreed there is a paucity of literature to answer that question."
Discussion
"So my view is that the very early administration of anti-coagulant likely induced more wound bleeding than if it had not been given, therefore the production of a bigger wound haematoma than would otherwise have been the case.
Mr Tolias found an organised clot. So a haematoma is generally an organised clot. It is fairly solid and can exert mass effect. Not necessarily liquid active bleeding. So my view is a clot formed in the early post-operative period and must have been clinically silent, and then continued to ooze or grow or it is not entirely clear why some haematomas present in a delayed fashion, but presumably some more mass effect, might have discussed potential other mechanisms, but then presented in a delayed fashion at approximately 40 hours."
Thus it seems to me to be likely that the giving of chemo-prophylaxis within about three hours of surgery caused or at least materially contributed towards the formation of the haematoma at L2 4. But for the giving of the chemo-prophylaxis at the time that it was given, I find either there would have been no haematoma or, probably more likely, the haematoma would have been significantly smaller and would not have impinged on the dura compressing it, as Mr Tolias found when he re-operated on 29 June 2013.
"Q: Of course it is reasonable to consider all sorts of options before surgery. But here, despite those unusual features, it is agreed between you and Mr Leach that the most likely cause was the compressive haematoma?
A: I think in our joint statement we do discuss this and I think we came to the view that Mr Leach felt that it was a majority haematoma with some inflammation and I felt that it was haematoma with a significant component of inflammation."
Thus, Mr Cadoux-Hudson conceded that the haematoma which formed has caused or made a material contribution towards Mrs Lesforis' neurological deficit, albeit in conjunction with inflammation.
Issue 2: was it negligent to delay intervention after 14.30 until surgery at midnight?
i) The timing: it was unusual for such a response to occur some 40 hours after the operation;
ii) The absence of severe pain which was very unusual;
iii) The form of presentation being wrong for a haematoma: thus, if it were a new bleed, it would be expected to be a progressive lesion and the loss of two motor nerves in isolation would not be expected without further loss of motor, sensory and autonomic nerves;
iv) The deficit appeared to be at the wrong level for a haematoma: the haematoma visible on CT scan was at L1/2 and the implicated level, L5/S1, was clear of compression.
In the circumstances, Mr Tolias took a considered and reasoned decision not to re-operate immediately, but to give steroids and see whether treatment for inflammation alleviated the situation and gave Mrs Lesforis some recovery. However, once it became clear, at about 10pm, that the steroids were not having the desired or any effect and that Mrs Lesforis' condition was essentially unchanged, he then re-operated.
70. On behalf of the Defendant, Mr Havers QC submits that, in the above circumstances, this was a consultant surgeon who was doing his very best for his patient in the circumstances. These were the considered decisions and actions of a very experienced and expert consultant, not merely the actions/decisions of a junior doctor. In so far as this is a case which concerns a consultant's clinical judgement and decision making, that deserves great respect. He reminded the court of what was said in Maynard v West Midlands Regional Health Authority [1984] 1 WLR 634 at page 638 E:
"A case which is based on an allegation that a fully considered decision of two consultants in the field of their special skill was negligent clearly presents certain difficulties of proof. It is not enough to show that there is a body of competent professional opinion which considers that there was a wrong decision, if there also exists a body of professional opinion, equally competent, which supports the decision as reasonable in the circumstances. It is enough to show that subsequent events show that the operation need never have been performed, if at the time the decision to operate was taken it was reasonable in the sense that a responsible body of medical opinion would have accepted it as proper. I do not think the words of Lord President Clyde in Hunter v Hanley [1955] SLT 213, 217 can be bettered:
"In the realm of diagnosis and treatment there is ample scope for genuine difference of opinion and one man clearly is not negligent merely because his conclusion differs from that of other professional men The true test for establishing negligence in diagnosis or treatment on the part of a doctor is whether he has been proved to be guilty of such failure as no doctor of ordinary skill would be guilty of if acting with ordinary care "
I would only add that a doctor who professes to exercise a special skill must exercise the ordinary skill of his speciality."
Mr Havers QC submits that this is precisely the situation here: not only was Mr Tolias exercising his skill and judgment as a neurosurgeon but he was also enjoying the support of his colleagues and he now enjoys the support of Mr Cadoux-Hudson. Thus, he submits that there is a responsible body of medical opinion which did support Mr Tolias' decision-making at the time and continues to support it at trial.
"Although the great majority of stones do pass without surgical intervention, what happened in this case must have been a foreseeable risk. In my judgment the patient should have been referred to the Middlesex Unit as planned. The problem did not resolve itself as hoped by the end of the week of 23rd January. It appeared to do so as a result of the shortening of the Yate's drain but this assumed that the stone had passed through the system when in fact it had not In short the surgical team took an avoidable risk. It was bad luck that the retained stone did not pass, as it was expected to do, and as the sensation of the bile leak through the drain seemed to indicate that it had. The patient should have been sent for the proposed ERCP at latest during the week beginning 31st January despite the modest risk involved in the accompanying removal of the stone endoscopically (or even by further laparotomy)."
In the Court of Appeal, Beldam LJ commented on the above passages as follows:
"In these two passages the Learned Judge appears to hold that the deceased should have been referred to the Middlesex Unit even though the problem appeared to have resolved itself because in the event it was shown that the stone had not in fact passed through the duodenum. But the question for the Learned Judge was not whether the risk could have been avoided if the deceased had been sent for ERCP, but whether Mr Wellwood and Mr Bursle in deciding not to send the deceased for ERCP when the fistula appeared to have closed displayed such lack of clinical judgement that no surgeon exercising proper care and skill could have reached the same decision."
Having considered the evidence, Beldam LJ went on to say:
"In my view, therefore, the question whether Mr Wellwood and Mr Bursle were at fault in failing to refer the deceased for ERCP, although the condition appeared to have settled, could not be determined by finding that the stone had not passed and that therefore they had made an assumption which was wrong. The question was whether, on the evidence, it was reasonable for them to take the view that the condition had settled, and whether it was in accordance with a practise accepted as proper by a responsible body of medical opinion not to refer the deceased for ERCP at that stage and in those circumstances. In this case the allegations of fault with which the Learned Judge had to deal called into question the fully considered decision of two surgeons in a specialist field of surgery in which they were skilled and experienced. Their decision was endorsed as being in accordance with a practise accepted as proper within the profession by an eminent surgeon practising in the same field. There was evidence that the specialist unit which would have conducted the ERCP examination also considered the decision a proper one. The fact that two other distinguished surgeons were critical of the decision, or that the decision ultimately turned out to be mistaken, does not prove that Mr Wellwood and Mr Bursle fell short of the standard of care to be expected of competent surgeons."
MRI Scanning
Conclusion
